Right from the start, it's essential to clarify the definition of obesity to dispel any misinformation and, honestly, to understand where you stand on the issue. Everyone knows of someone who has had a successful weight loss journey - so why can they do it and everyone else cant?
The most frequently cited definition states: Obesity is a chronic medical condition characterized by pathological (i.e., harmful) adipose tissue or fat cells that impair health. If you live in a larger body but do not have adipose tissue impairing your health, you do not have obesity. It is not determined solely by weight or BMI (more on BMI later). Understanding this principle allows you to sift through 90% of the misinformation prevalent on social media. The "healthy at every size" philosophy remains valid, provided your health is not impaired by adipose tissue. Those advocating that diet and exercise are the solution are not incorrect, but this approach is unlikely to be effective for individuals with health-impairing adipose tissue. Get the definition right, and the rest becomes clear as mud.
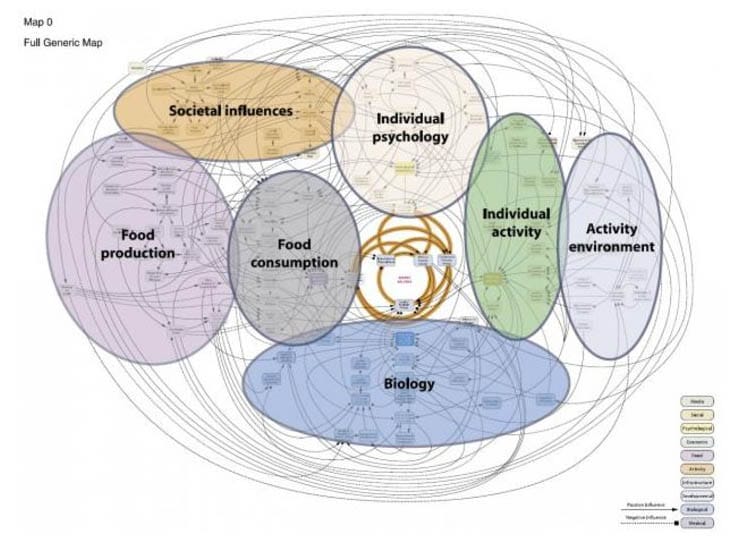
In the ongoing discourse on health, weight, and obesity, it's crucial to start with a clear idea of what we're discussing. I alluded to this in my last post about obesity treatments not being equivalent to weight loss which you can read here. The conversation around obesity is riddled with misconceptions, biases, and oversimplified narratives that fail to address the complex reality of the issue. It involves more than just having a Body Mass Index (BMI) greater than 30; it involves a complex interplay of our biology, metabolism, genetic predisposition to defend our body's highest weight, and our modern food environment (See obesity systems map below).
Let me explain why losing weight is challenging when you have obesity (also known as adiposity that impairs health).
Obesity and being overweight are distinct diseases, not just in the scale but in their implications for health. The core issue lies in adipose tissue—commonly known as body fat—and its effects on every organ system in our body. Unlike the "storage depot" it's often mistaken for, adipose tissue, especially around our abdomen and internal organs, is an active endocrine organ. An endocrine organ is an organ that produces hormones and releases them into the bloodstream to travel throughout the body. This can affect our heart, brain, kidneys etc. The dysfunctional adipose tissue required for a diagnosis of obesity does precisely that. Its impact is profound, through multiple mediators, many of which are pro-inflammatory and lead to the majority of obesity-related problems like heart disease and fatty liver. The hormones released by adipose tissue significantly influence the brain and its appetite system. For instance, dysfunctional adipose tissue causes leptin resistance, a condition where the brain doesn't receive signals of fullness effectively, making people with obesity feel hungrier than those without. Advising someone who is inherently hungrier to eat less is unlikely to be a sustainable solution. This hunger affects concentration, work, and sleep, leading to a self-defeating prophecy. Additionally, when you have obesity and lose weight, you also burn fewer calories, a mechanism our bodies use to ensure survival. This can lead to a weight loss plateau even when adhering to a low-calorie diet. Our brain's appetite system also regulates the pleasure we derive from food, not just hunger. This response is genetically predetermined, making some people more susceptible to their food environment than others. Reducing calorie intake naturally leads to more frequent thoughts about food.
This is obesity.
If you consume excess calories (for many different reasons) and gain weight, merely reducing those calories does not mean your body will allow your weight to go back down. Your pathological adipose tissue and biology will work against you, and *most people will regain weight back to their natural highest weight. What can you do to counter these biological processes, which are more pronounced in some than others, and are designed to protect our bodies? The options are to eat even less—despite being hungrier and thinking about food more—or to exercise more. This is the only way to combat obesity through lifestyle changes alone, and as you can see, it's a diminishing returns situation. The effort required to maintain weight loss increases over time, leading many to revert to previous behaviors, causing the weight to return. Genetics play a significant role in this process, influencing both food intake and energy expenditure, making weight largely beyond individual control. Let me say that again, in obesity, your weight is largely beyond your control. It's important to note that we're discussing adiposity that impairs health and individuals with a genetic predisposition, not everyone who gains weight or carries extra weight. This means you can gain and lose weight, then gain it again and struggle to lose it despite the same behaviors; this is obesity. This is not an argument against nutrition and exercise; it's an effort to understand why these measures alone are not effective treatments for people with obesity but remain important for everyone.
Is obesity a disease or a symptom of another problem?
Well, we gain weight for lots of different reasons. Medications, eating too much, less exercise. Understanding why this happens is crucial to prevent further complications. However, if you have a biological predisposition and genetic makeup that leads to the accumulation of dysfunctional adipose tissue when you gain weight, the reason behind the weight gain becomes less significant, you will have a harder time losing it and you will likely be at risk of health issues because of it. This is obesity. While many focus on preventing obesity through diet and exercise as a way to allocate healthcare resources efficiently, what about those who are already struggling? Instead of only treating the myriad health issues caused by obesity, shouldn't we also focus on treating the obesity itself? Some people manage to lose weight and keep it off, but others do not. For those who don't — 1 in 4 adults worldwide — treatment is necessary. Such treatments address the biology and hormones that influence our appetite system, the same hormones that dysfunctional adipose tissue alters to increase hunger when you try to reduce calories (e.g., GLP-1 medications like semaglutide and tirzepatide). Behavioral treatment is also crucial to help us understand and assess the modulators of appetite, the reasons behind our eating habits. Sleep, stress, and mood often drive us to eat to feel better. GLP-1 medications are frequently mentioned as a way to "reduce food noise," and contrave, another Health Canada-approved medication for weight management, targets just that. It's important to recognize that the food industry has exploited this natural human behavior of seeking pleasure, creating foods that perfectly fulfill this desire. As a result, we struggle with controlling our food intake, especially in an environment abundant in food and high in stress.
This definition of obesity challenges the oversimplified adage that weight loss is merely a psychological battle, a test of willpower. Willpower, contrary to popular belief, is not an infinite resource. The biological imperative to restore energy reserves, especially after periods of caloric restriction, eventually overrides conscious efforts to maintain weight loss. This inevitable physiological response underscores a critical truth: if you struggle with weight, it's not your fault.
This perspective, however, is not universally accepted, leading to a pervasive culture of blame and misunderstanding. There are multiple assumptions that I have come across for anyone who lives in a bigger body 1)they must have health issues 2) they must want to lose weight 3) they must be over-consuming calories because they “can’t control” themselves, or they dont want to exercise. These assumptions are also why most people with obesity have internalized bias - they have accepted that they do not deserve the same respect as those without obesity because they believe these assumptions are true. (Lots more on this later, its so so important to break down) Here’s the problem - despite what you might think, you can’t actually see obesity. You can see adipose tissue. But can’t see if adipose tissue impairs health. All you can see is body size. Stick to the definition, and the rest will become clear.
Maybe we should just skip over using the word obesity at all. Let’s just treat the adiposity so that we can finally win at treating diabetes, heart disease, cancer, fatty liver etc etc. It seems like everyday someone will debate me on why medications should not be used for obesity, yet we have 52 medications in our diabetes tool box. I’ll be the first to say we are not succeeding at improving rates of diabetes despite these treatments. But, I think the pendulum has swung way too far in favour of medications without behaviour change. We need both. If your control of eating is improved but you haven’t improved your relationship with food, the treatment will not be successful.
In addressing the complex issue of obesity, it's imperative to move beyond simplistic narratives of blame and individual failure. Recognizing adipose tissue as an endocrine organ sheds light on the physiological challenges involved, underscoring the need for compassion, comprehensive care, and systemic change. This is obesity.
Shifting the conversation from judgment to understanding, from blame to support, is essential. By sticking to the definition, the rest becomes as clear as mud.